By Lana Sweeten-Shults
GCU News Bureau
Joey Hermosillo knew something wasn’t right. He didn’t quite feel like himself.
He felt like something was waiting.
Something lurking.
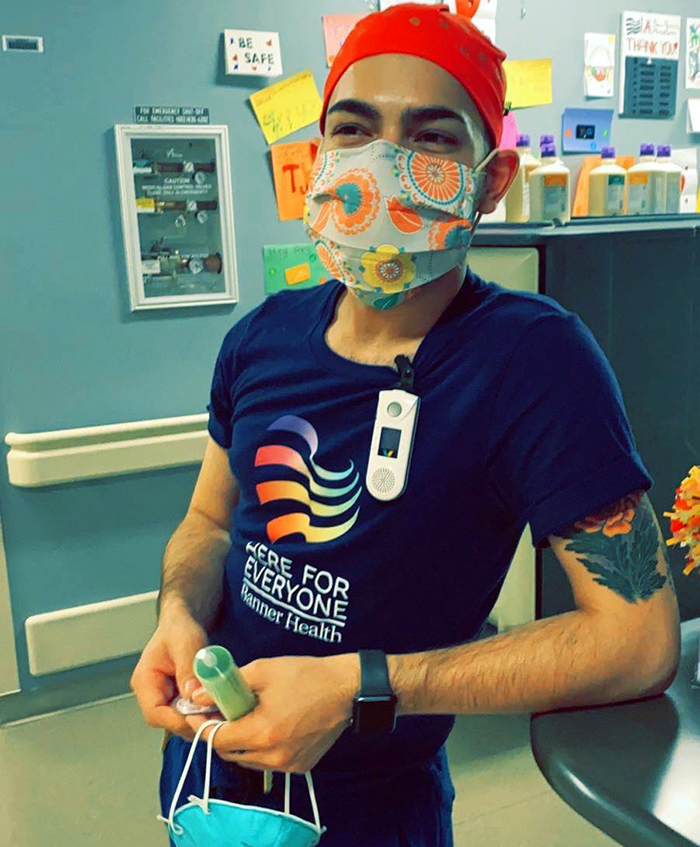
But the Grand Canyon University alumnus and charge nurse at Phoenix’s Banner University Medical Center in Phoenix ignored his headache and, after a sleepless night, could only think of one thing: returning to work to help his fellow nurses and patients win the COVID-19 fight.
So he downed some Ibuprofen, took his temperature – 98.7 degrees Fahrenheit -- and started his shift. But by the middle of it, he felt exhausted.

His temperature after lunch: 99.6 degrees.
That’s when he knew he needed to go home. After a nap, he took his temperature again: 101.8 degrees.
“My whole body hurt, and I had chills,” said Hermosillo, who would find out after a trip to urgent care and a five-day wait for test results that he had contracted COVID-19.
More than 108,600 confirmed COVID-19 cases have been declared in Arizona as of Wednesday, according to the Arizona Department of Health Services, and more than 3.11 million cases exist in the United States.
“I felt like I had a cold … but this ‘cold’ felt like no other – and then some. I had a headache, body aches, chills and fever. For me, the body aches stood out. They were the strongest I had ever felt. I would move my body in bed, and it would hurt from head to toe.”
But not even that could stop him from returning to work.
Just 10 days after being quarantined with a mild case of the coronavirus, he was cleared to return to Banner University’s Trauma/Surgical Intensive Care Unit.
It’s exactly what he did, no hesitation.
“The day I was cleared for work, I almost picked up a night shift,” he said. “I was SO ready.”
Since he returned to work in early July, Hermosillo has put in a week of back-to-back shifts.
That relentless drive to help others was apparent even as a student at GCU, where he switched his major three or four times before going into pre-med and, for the first time, really loving his classes.

It was when he started working full-time as a certified nursing assistant to beef up his medical school application that he realized he wanted to be a nurse.
“Just watching them, what they did for the patients throughout the day, their interactions with the doctors, all the responsibilities that fall on them. I said, I really like this role where you are the epicenter of every patient’s hospital stay,” Hermosillo said.
“You are the one that has your hand in every little pot that goes into a patient’s whole stay. I think that’s so cool, the power that it has, the responsibility that it has.”
Looking back, he thinks the reason he bounced around so much was because “I was scared of the schooling … I was scared it was going to be too hard.”
And it almost was.
But those difficulties prepared him for a challenge he never could have imagined – fighting a daunting global pandemic.
Hermosillo, a native of Chihuahua, Mexico, grew up in west Phoenix, practically in the shadow of GCU. It felt right to him to stay in the neighborhood, close to family, and become a Lope.
Once he did, he didn’t have time to do much of anything beyond school and work.
“I worked three nights of the week, then I would go to school during the days," he said. "There were days I’d do 30- or 32-hour days awake.”
What made Hermosillo’s situation even more difficult was that he’s a recipient of the Deferred Action for Childhood Arrivals, or DACA, which allows some illegal immigrants brought to the country as children to become eligible for a work permit.
“My freshman year (2012) was when DACA came out. I applied and got my permit. As soon as I did that, I started working,” he said, but acknowledges, “In the blink of an eye … it can get taken away.”
That disconcerting thought is always in the back of his mind as he continues the work he started in the College of Nursing and Health Care Professions.
Soon after graduating in 2016, he moved into trauma care.
Working with trauma patients is intense, he said: “They don’t come in just with the head bleed, or it’s not just the gunshot wound. You’re not just taking care of the hole that the gun or the bullet made. There are SO many other things that come with taking care of a trauma patient or even a sick surgical patient. There’s so much involved; you have to look at the whole picture.”
While his primary responsibility is in the Trauma/Surgical Intensive Care Unit, he also rotates through the COVID-19 areas of the hospital as needed.
The Arizona Department of Health reported that deaths in the state are approaching 2,000 and that 91% of adult ICU beds were in use as of Wednesday as Arizona has become one of the hot spots for the spread of the virus.
Hermosillo sees those statistics firsthand.
In February, Arizona officials saw what was happening in New York and began to prepare. By March, Gov. Doug Ducey mandated hospitals to increase their ICU capacity by 50%.
“We made beds where we had to,” Hermosillo said of Banner University’s coronavirus units, which quickly became known as Camp COVID.
Everyone who arrives at the hospital is treated as if they were COVID-19-positive, and medical personnel think of themselves as having been exposed.
“It kind of keeps us on our toes, where everyone’s protecting themselves and covering themselves and hand-washing,” he said.
When there’s a call to the trauma bay, Hermosillo and the rest of the medical team fully gown-up.
"It’s a gown, two to three masks, hair covering, shoes. You’re immediately hot. You’re so uncomfortable,” Hermosillo said. “No one can hear each other behind the two or three masks you’re wearing. You’re so sweaty and hot. Everything’s happening and it’s so quick.”
Hermosillo said medical personnel don’t know if someone they’ve treated is COVID-19-positive until days afterward. And even with asymptomatic patients, “Two or three days later, this patient in the regular ICU is having a fever, their respiratory status is declining, and then we start to think maybe it’s COVID. But at that point, that patient already has been on the floor for three days. Multiple people have been in and out of their room.
"So even if I’m not in the COVID ICU every day for my shift, the exposure risk, the potential to come into contact with someone without even knowing it, is just as high.”
Beyond that, Hermosillo said ICU nurses are caring for three patients at once compared to two patients max before the pandemic. More medical personnel are starting to burn out or, like Hermosillo, they get sick themselves.
“We’re not used to taking care of more than two very sick ICU patients," he said. "Whenever I’m charge nurse, I always feel like I’m begging half the time for people to pick up extra shifts. … The other day I was barely waking up. It was 8 a.m. and I had like eight calls from the hospital. They were that desperate.”
He and his fellow nurses worry, too, about how the pandemic might affect those considering becoming a nurse. Will they still want to become nurses? Will they think like Hermosillo did, that it would be too hard? Or will they want to become a nurse even more than before?
If there’s anything he wants to convey from his experiences, he said it’s to encourage everyone to wear masks in public spaces, pay attention to their bodies and start quarantining or seeking a test if they have symptoms that warrant it.
“Truly no one will know or understand what challenges we have had to go through recently to make ends meet in providing care unless you are in it.”
Despite fighting COVID-19, and in spite of all the challenges of the past few months, “this is definitely where I want to be,” Hermosillo said.
No hesitation.
GCU senior writer Lana Sweeten-Shults can be reached at [email protected] or at 602-639-7901.
***
Related content:
GCU Today: Residency changes unmasked in face of COVID-19
GCU Today: No hospital? No problem: Nursing students go virtual














